Optimizing Mobility with Multiple Sclerosis Physical Therapy
Multiple sclerosis, a chronic immune-mediated disease affecting the central nervous system, often results in mobility impairment, among other neurological symptoms. Its onset typically occurs in young adulthood, making its progressive nature particularly challenging for those diagnosed.
As the disease progresses, motor functions can be compromised, frequently manifesting in gait difficulties and necessitating a lifelong adjustment to a changing physical capacity. Recognizing these challenges, physical therapy stands out as a proactive approach to enhancing mobility and quality of life for individuals with multiple sclerosis.
Focusing on strength, balance, and coordination, physical therapy tailors exercises and rehabilitation techniques to individual needs.
By supporting neuroplasticity—the brain’s ability to reorganize and form new connections—physical therapy aims to improve patient outcomes, helping those with multiple sclerosis maintain independence and manage physical symptoms more effectively.
Key Takeaways
- Optimizing mobility in multiple sclerosis involves individualized physical therapy strategies.
- Rehabilitation focuses on strengthening, balance, and gait training to enhance quality of life.
- Physical therapy leverages the brain’s neuroplasticity to improve overall function in multiple sclerosis patients.
Understanding Multiple Sclerosis and Its Impact on Mobility
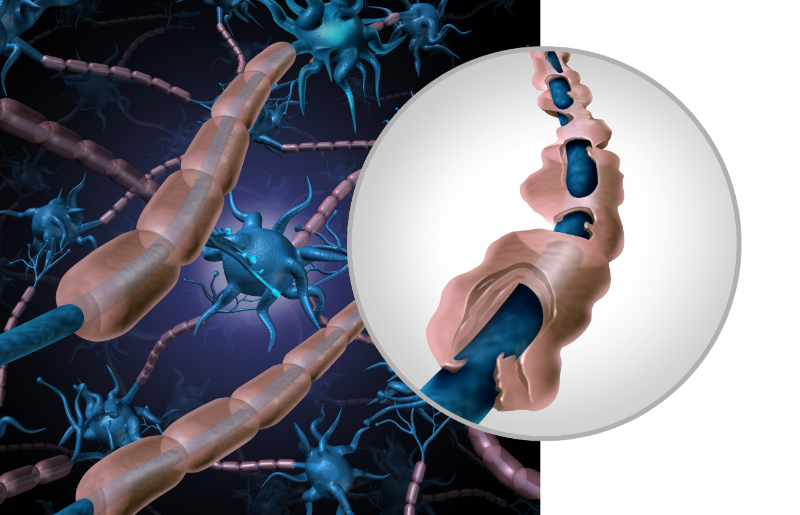
Multiple sclerosis (MS) is a neurological condition with significant implications for mobility, directly affecting patients’ quality of life.
As we explore the intricate relationship between MS and mobility, we focus on the pathophysiology leading to mobility impairment and the critical assessments used to evaluate mobility challenges in individuals with MS.
Pathophysiology of Multiple Sclerosis and Mobility Impairment
MS is a chronic autoimmune disease of the central nervous system (CNS) that disrupts the flow of information within the brain and between the brain and body. The disease is characterized by the immune system attacking myelin, the protective sheath covering nerve fibers. This results in communication issues, scarring or sclerosis, and permanent nerve damage.
There are two main types of MS: Relapsing-Remitting MS (RRMS) and Progressive MS (PMS).
RRMS is marked by episodes of new or increasing neurological symptoms, known as relapses, followed by periods of partial or complete recovery. In contrast, PMS involves a steady progression of disability without relapses.
Mobility disability arises as MS progresses, with symptoms like muscle weakness, spasticity, balance coordination problems, and fatigue contributing to reduced gait speed and walking difficulties.
Over time, these symptoms can escalate, limiting an individual’s ability to perform daily tasks and impacting their quality of life.
Physical Therapy Approaches for Enhancing Mobility
In managing multiple sclerosis (MS), we recognize that physical therapy is crucial for maintaining and improving mobility. Our focus is on evidence-based, individualized exercise interventions that aim to enhance muscle strength, coordination, and overall physical activity.
Importance of Exercise in MS Management
We understand the undeniable role of exercise in managing the symptoms of MS. Regular physical activity provides significant benefits in balance and muscle strength, which are often compromised in MS patients.
Engaging in resistance training and aerobic exercise, such as cycling, promotes fitness and neurorehabilitation. Moreover, balance training, including yoga, can be instrumental in preventing falls and enhancing one’s ability to perform daily activities confidently.
Tailored Exercise Programs for MS Patients
Our tailored exercise programs for MS patients address the unique challenges faced by each individual. Recognizing the variability in symptoms and progression of the disease, we design programs that incorporate strength training and balance exercises.
These programs might include:
- Neuromuscular Facilitation: Enhances movement patterns and muscle activation.
- Stretching and Mobilization Techniques: Improve flexibility and range of motion.
- Exercise Training Components: A mix of resistance and aerobic exercises tailored to the patient’s fitness level.
Exercise regimens are monitored and adjusted to match patients’ evolving needs, ensuring optimal outcomes are achieved safely and sustainably.
Incorporating Assistive Devices and Technologies
In conjunction with exercise programs, we also value the role of assistive devices and technologies in supporting mobility. Assistive devices—such as walking aids—are fundamental in providing stability and independence.
Moreover, new technologies like robot-assisted gait training offer innovative ways to rehabilitate walking patterns. By integrating these tools into physical therapy regimens, we enhance patients’ potential to maintain and regain mobility.
Maximizing Patient Outcomes and Quality of Life
In managing Multiple Sclerosis (MS), we focus on enhancing each patient’s quality of life. This entails meticulously addressing fatigue and muscle weakness alongside fostering a supportive community environment for comprehensive care.
Strategies for Managing Fatigue and Weakness
In our approach to managing fatigue, a primary concern in MS, we employ interventions such as:
- Structured exercise regimens: Tailored to individual capabilities, including strengthening exercises to combat muscle weakness.
- Energy conservation techniques: Encouraging patients to balance activity with rest, potentially utilizing the Fatigue Severity Scale to monitor and adapt to energy levels.
- Heat management: As heat can exacerbate fatigue, strategies like staying hydrated, using cooling garments, and regulating ambient temperature are crucial.
- Medication review: Referral to medical colleagues for the management of symptoms that may influence fatigue.
Building a Supportive Community Environment
- Safety promotion: Addressing home and community safety through fall prevention strategies and education on minimizing relapse.
- Disease management education: Empowering patients with knowledge to manage their condition, including recognizing signs of exacerbation.
- Network referral: Connecting patients to support groups and services within the community to bolster psychological well-being and HRQoL (Health-Related Quality of Life).
- Professional collaboration: Utilizing a team-based approach involving various healthcare professionals to ensure a coordinated and comprehensive plan.
Frequently Asked Questions
In our practice, we address common inquiries about optimizing mobility through physical therapy for those living with multiple sclerosis. These questions guide our tailored interventions.
What types of physical therapy are most effective for improving mobility in multiple sclerosis patients?
We integrate balance and neuromuscular facilitation exercises alongside stretching and mobilization techniques. Resistance and aerobic training are often essential components due to their efficacy in enhancing mobility.
What precautions should be observed during physical therapy for those with multiple sclerosis?
Patients must pace their activity to avoid fatigue and overheating. We closely monitor each patient’s response to exercise to adjust the intensity and ensure safety.
How can gait abnormalities be addressed through physiotherapy in multiple sclerosis cases?
We employ strategies such as strength training and task-specific exercises. These can help correct gait irregularities and improve walking patterns.
Which exercises are considered safe and beneficial for patients with multiple sclerosis?
Exercises tailored to the individual’s capabilities, such as swimming or seated exercises, are beneficial. They reduce the risk of falls while promoting muscle strength and cardiovascular fitness.
How does physical therapy contribute to managing spasticity in multiple sclerosis?
Through regular stretching and strengthening exercises, we are able to help maintain muscle flexibility and reduce the severity of spasticity. This aids in preserving mobility and daily function.
What are the contraindications for physical therapy in the management of multiple sclerosis?
Contraindications can include acute relapse, severe fatigue, or recent injury. We always perform a thorough assessment before recommending a physical therapy regimen.